Technical and scientific discoveries and innovations are happening at a tremendous rate. Social attitudes and morality have also undergone huge shifts in just the past two generations.
Try this mental exercise. Imagine virtually any community in the 1950s and then fast-forward to the present. Almost nothing will have remained untouched. The geography and enduring elements like architecture may be substantially similar, but the automobiles, any technological item, even the demographic characteristics of that community will be largely different. Even the most basic social laws like those defining marriage or protection for the right to life before birth have changed alarmingly. We are living through radical technological and social revolutions moving at breakneck speed.
It feels like our societies have been catapulted into a strange utopian social science experiment. A person coming of age in the late 1950s has a substantial chance of being alive today thanks to the average life expectancy extending to great old age today. This person born into a family with his/her father and mother married to each other as a societal norm sees a very different picture today among his/her grandchildren’s generation. That the gender of every human was either male or female and heterosexual normativity did not pose any question at all not so long ago. There were no headlines discussing a “woman” who was born male but then took hormones or had sex-change surgery and now demands to compete in female athletic events.
Finally, the rights of parents to educate and raise their own children were universally acknowledged. Only the most severe forms of abuse were considered grounds for separating children from their parents.
Rights of Parents, Guardians of Their Children
Modern child-rearing combines several phenomena. Children increasingly often remain dependent on their parents for years beyond their legal maturity. The average age of mothers and fathers at the birth of the first child has climbed steadily while conversely global fertility rates have plummeted over the past few decades. These older and older parents are faced with children who remain financially dependent for longer periods of time as they pursue years of higher education and even sometimes move back home after unsuccessfully attempting to launch their independent work lives.
The old truism about the “empty nest” is less and less of a common phenomenon.

Society also intrudes more often into the sanctum of the home and the authority, responsibilities, and rights of parents vis-à-vis their children. Schools routinely deny the right of parents to exempt their children from mandatory sex education classes that contradict the morals and religious beliefs of these families. Government-sponsored social agencies have taken children away from their parents, not for any kind of physical abuse, but rather for educating their own children with their conservative religious views. Hospitals and health authorities sometimes make decisions regarding sick babies that contradict the wishes of parents, even in cases where their status as the legal guardians for these minors has not been rescinded.
It is important to discuss this topic of the modern legal conflicts between institutions and parents in health care decision-making for children. It raises a serious issue of medical ethics. Who has the competence to decide in concrete medical cases? The consensus view among ethicists and in legal norms is that an adult with a sound mind has the legal right to decide the medical treatments they will or will not undergo, with the exception of emergency situations, as part of informed consent in medicine. In the case of a child, and particularly when it comes to babies, a legal guardian or guardians have this power. Almost universally, the biological parents are entrusted with this role. They are deemed to have the best interests of their child at heart. Legal guardians for children who are not their parents can be appointed and indeed the rights of parents can be legally terminated if either or both the mother or father have demonstrated a lack of regard for the safety or well-being of the child.
All of this is theoretically straightforward and in fact is hardly ever challenged. There may be some disagreement in particular cases as to a parent truly being “unfit” or not, but the general view that parents will almost always have the best interests of their little boy or girl at heart when making medical decisions in a hospital setting is uncontroversial. Yes, there are ethically wrenching situations like where parents refuse to allow a needed blood transfusion for a child because they are practicing Jehovah’s Witnesses. Thankfully, these cases are rare.
I will not explore in depth developments in children’s rights. A modern movement has achieved international recognition for increasing the autonomy rights of children at the expense of the rights of parents. This vast topic includes both recognition of some true rights and some clear usurpation of parent’s rights, particularly by institutions acting on behalf of minors. The main thrust of my argument here, however, concerns medical decision-making for infants and therefore is largely out of the domain of the new children’s rights debate.
Medical discoveries and technological advances are increasingly creating more ethical conflicts involving very sick babies. Throughout most of human history infant mortality was extremely high. It was one of the main limiting factors of human population growth. Perinatal mortality, the death of the fetus or newborn in the first week after birth, was particularly high. Modern medical science has reduced perinatal mortality rates substantially. It is still true, however, that most children who die do so in the first year of life. A modern ethical challenge is the increasingly frequent situation of a very sick patient who cannot be cured by current medical science but who can be kept alive by a combination of therapies and machines at great cost.
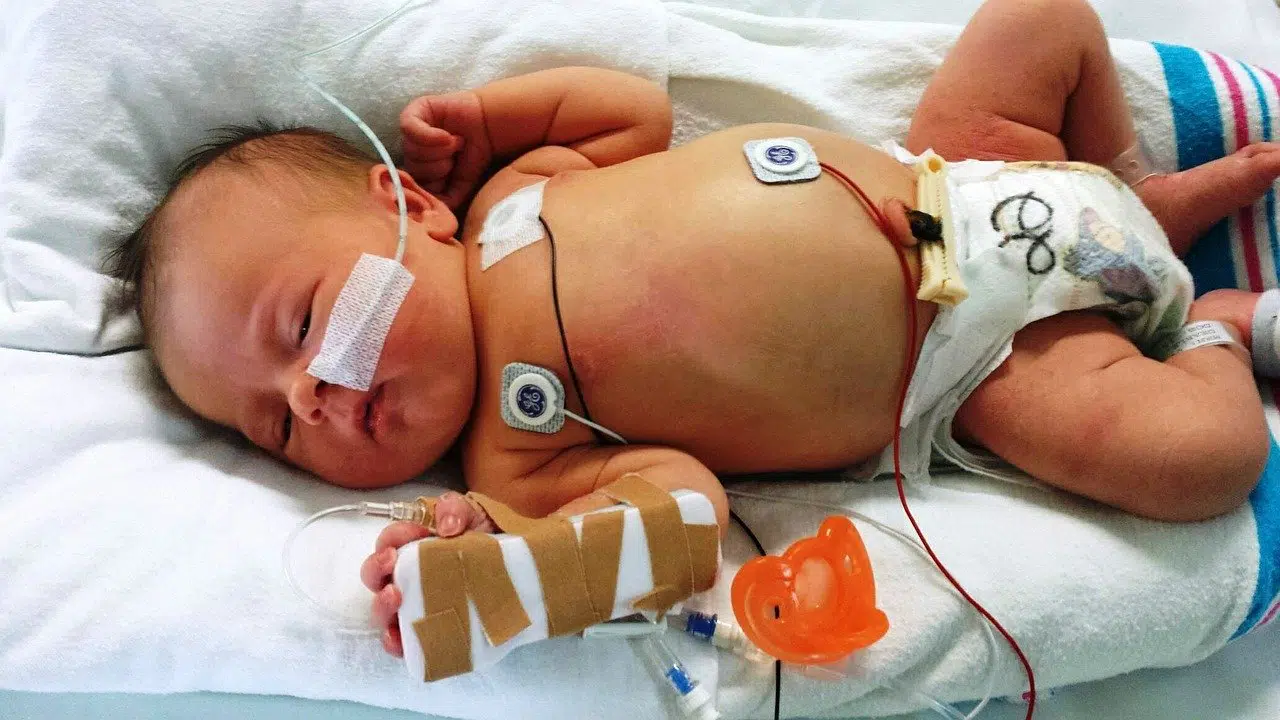
It is an extremely ethically uncomfortable position for a medical professional to have a patient who has a very poor prognosis for recovery, or even conscious living, but who can be prevented from dying for an extended period of time. These patients can fall into a kind of limbo category where it is unclear where their true best interests lie. Should everything be done to preserve their lives while hoping for a “medical miracle”? Is it more merciful and just to disconnect them and allow them to die? Is there a middle ground position that is preferable?
The Morality of Withdrawing Care
The Catholic Church offers an analytical tool in taking these decisions. She makes a distinction between “ordinary” and “extraordinary” means in health care. Very simply stated, ordinary means are always morally obligatory for patients while extraordinary means are optional.
Of course, the devil is in the details. What is ordinary or extraordinary? Because of medical progress what was clearly extraordinary many years ago, like renal dialysis, has largely become ordinary care. It may still be the case, however, that in a poor country dialysis is still extraordinary because of its lack of availability. There is also a strong subjective element on the side of the patient. Some people are extremely distressed or suffer terrible side effects from treatments like chemotherapy that have become quite ordinary in cancer care. In such circumstances, a good case can be made that it is not unreasonable to consider the treatment as extraordinary because of the burdens it imposes, and therefore that it is not ethically obligatory.
The Catholic Magisterium or teaching authority has provided much more explicit guidelines for ordinary care. Nutrition and hydration, whether by natural or artificial means, are to be considered ordinary care. The reasoning for this is straightforward. All human beings require food and water to live. To cut off these basic necessities is a form of passive euthanasia.
An exception even to this rule is admitted. If the patient is in the final days of life, and withdrawing a feeding tube or accepting that the person no longer wishes to be hand-fed will not lead to their deaths, it may be less burdensome for the patient and morally licit to allow them to forgo nutrition. It is frequently observed that in a patient who is slowly dying a point occurs where his or her body simply shuts down and no longer absorbs food. Hydration is a more acute need than nutrition, and it is rare that the same criteria for it to become an extraordinary means apply. Even in those cases, moistening the lips and skin of the dying person are ordinary care as well as the other most basic measures to keep the dying person comfortable.

The Church teaches we must provide ordinary care.
Another crucial aspect of this ordinary vs. extraordinary means distinction involves the common good. Societies and families have a duty to provide ordinary care to their members. They should also provide access to health care, although they are not required to offer every form of extraordinary care available. Difficult decisions have to be made concerning health policy since available resources are by definition finite.
On the other hand, the demand for health care services generally far outstrip even the most generous health plans and state health services, particularly for acute pathologies. The fear of imminent death can lead individuals or their legal guardians to extreme decisions. When a person is spending their private wealth to pursue experimental or burdensome and costly treatments that have a very low chance of success, this will, in most cases, fall under the category of licitly choosing extraordinary means. More frequently, however, the issue is whether society is willing to cover the costs of these therapies, and that is much less easy to decide. It is certainly not ethical to allow a very small number of patients to consume societal health care resources that could be used to save many more lives. Where exactly to draw the line is a thorny issue that requires the input of ethicists and specialists in several fields.
The problem is even more difficult when the patient is a tiny innocent baby. Imagine your desperately sick newborn in a hospital Neonatal Intensive Care Unit. It is almost unbearable. Most parents will want every possible medical means used regardless of cost or chances of success. In some cases they may become irrational on the topic and even abusive of medical staff that refuses to comply with their wishes. Spiritual and even psychological support is needed in most cases. In the most exceptional scenarios an independent legal guardian for medical decision-making may need to be appointed. Great care must be exercised, however, as the sacred bond between mothers and fathers and their children; the rights of parents are not something that can be violated except for a particularly extreme situation.
The Push for Patients’ Rights
Strangely, in this area, trends seem to be going counter to the general direction of bioethical consensus.
Over the last few decades a strong push for greater patient autonomy has replaced the previous paradigm of medical paternalism. It is something of a cliché to refer back to a past period when the doctor told the patient what would be done and the sick person simply had the duty to acquiesce. Today informed consent is the gold standard. Medical professionals are required to explain treatment options as clearly as possible and allow the patients to decide what they want.

In its most extreme form this modern view is that the patient decides and the doctor is required to carry out his wishes. It is an illogical position to take since in the name of the autonomy of the patient the professional autonomy of the health care worker is sacrificed. This also helps to explain why among medical personnel conscientious objection has become such a prominent topic of ethical discussion.
Rights of Parents Violated: Examples in the News
So, while there is generally higher respect for patient autonomy and informed consent today, these rights appear to be problematic at times for parents as legal guardians in medical matters for their sick children. The spectacular cases that make international headlines such as those of Charlie Gard or Alfie Evans are certainly rare but remain disturbing. An in-depth study of the number of these cases would certainly be necessary to have a better idea of the scale of the problem today. We can nevertheless benefit from a brief analysis of these two cases.
Both Charlie Gard and Alfie Evans were suffering from severe conditions that required extraordinary medical care to continue living. In both cases the parents wished to explore further medical care for their children and came into conflict with the doctors and hospitals caring for their sons. Both cases arose in Great Britain. These two conflicts dragged on and went through extensive court cases on multiple levels of jurisdiction. Regardless of the scientific merits of the medical opinion defended by the institutions in each case that further care was futile, the most shocking aspect of Charlie Gard’s and Alfie Evan’s situations was that the hospitals refused to allow them to be discharged at the request of the parents.

It is a clear violation of patient autonomy to allow a patient to be voluntarily admitted but then to refuse to discharge that patient when other treatments that the hospital in question refuses to provide are chosen. In effect, the patient is being held prisoner in the hospital. In the Alfie Evans case, a police officer was even posted outside the baby’s hospital room to prevent the parents from exercising this right.
Even worse, the hospitals insisted on and obtained court orders to disconnect the respirators of the infants in the clear knowledge that this would lead to rapid death. One can only imagine the desperation of fathers and mothers, not convinced that nothing more can or should be done, who are physically prevented from exploring other medical options and helplessly can only look on as their child dies.
Charges of cruelty and human rights violations are not amiss, particularly when even the request of Charlie Gard’s parents that their son be allowed to come home to die was denied. The Bambino Gesù hospital in Rome run by the Church offered to provide free medical care to both boys. In neither case were there any credible charges that the parents did not sincerely want what was best for their sons. It appears they were the victims of a medical and legal establishment that refused to honor the most basic autonomy right of patients to seek out the best care they could find. It should be noted that the economic ethical arguments regarding resources did not apply to the final decisions to refuse to discharge the children since the parents had found alternative providers and charitable donations that would not cost the British tax payers anything.
In the United States so-called “futile care” laws have passed in many states to apply in cases where medical institutions want to cease extraordinary medical treatments and the patients or their representatives refuse to accept this decision. It is not the case, however, that they refuse to allow the patients to be discharged. Accusations have been leveled, nonetheless, that at times hospitals refuse to admit patients discharged by others on grounds of the futility of further treatment. This problem can equally leave patients with no options except to acquiesce to having their life-support unplugged and dying where they are.
Conclusion
We should take stock of the incredible transformations of our societies in recent years. Saint John Paul II warned of a rising Culture of Death in our world. He defended the Church’s vision and the natural law on marriage, the family and the duties and rights of parents. The modern turbulence of technological changes combined with changing morals make resolving medical ethical issues ever more complicated today. It is simply unacceptable that most patients should benefit from the recognition of enhanced autonomy rights while the rights of parents can be easily overruled or negated in the medical care of their children. In a world where economic difficulties and skyrocketing medical costs are a harsh reality, it seems inevitable that even more restrictive medical rationing will be implemented.
As traditional morality is increasingly disparaged and violated in law and medicine, it is hardly surprising that parents can face a battle to have their rights respected. The tragedy is that sick little children risk being the victims of a cold and unfeeling modernity. It is vital that the consciences of our contemporaries and their hearts be touched and enlightened.
No, parents are not always right, but they deserve to be given, not only the benefit of the doubt, but also our moral and spiritual support when faced with the tragedy of a grievously ill baby.

Related Content
One of the world's leading experts on the international pro-life movement, Dr. Meaney received his PhD in Bioethics at the Catholic University of the Sacred Heart in Rome in 2015, writing on “Conscience and Health Care.” He was named an honorary visiting professor at Benedict XVI Catholic University in Trujillo, Peru.
Dr. Meaney's work has been featured in publications such as Crisis Magazine, National Catholic Bioethics Quarterly, The American Spectator, Inside Catholic, National Catholic Register, and LifeSiteNews. He also appeared in the pro-life documentary “Silent Fall,” and is featured in HLI’s documentaries which debuted on EWTN “Central and Eastern Europe: A Return to Life” and “Central America and Mexico: Fighting for Life, Faith and Family.” After many years as HLI's Director of International Outreach and Expansion, he became President of the National Catholic Bioethics Center in 2019.














