The use of condoms is considered normal, almost compulsory, for many people engaging in sex today, whether married or unmarried. Of course, pro-lifers and Catholics oppose this unnatural device on the moral level. It not only disrupts the mechanism of transmitting human life in the most direct way possible; it also encourages promiscuity with false promises of “preventing pregnancy” or diseases.
But even on the practical level, condoms don’t do what they are meant to! The condom “failure” rate (meaning the possible permission of natural pregnancy) is high, and the latex balloon carries with it a host of other practical problems.
(A note: this article uses scare quotes for phrases like “prevent pregnancy,” “failure,” and others, because these are talking points from the contraceptive worldview that divorce sex from procreation as a natural end.)
How effective are condoms? How effective are they at “preventing pregnancy”? The answer to these questions: not very. In this article, we’ll cover the following points about the ineffectiveness of condoms:
- Condom “failure” rate is high
- Condoms do not “prevent pregnancy” over time
- Condom promoters use irrelevant evidence
- Condoms haven’t delivered statistically
Let’s begin.
1. Condom “Failure” Rate Is High
The male condom is the most commonly used barrier method of contraception in the world. But how effective are condoms? According to mainstream scientific sources, their efficacy has been grossly overstated by condom promoters. After the use of just 10, the probability of at least one “failure” is 46.51%, according to calculations done by Human Life International based on data from the authoritative Contraceptive Technology (21st Edition, 2018) and other sources.1
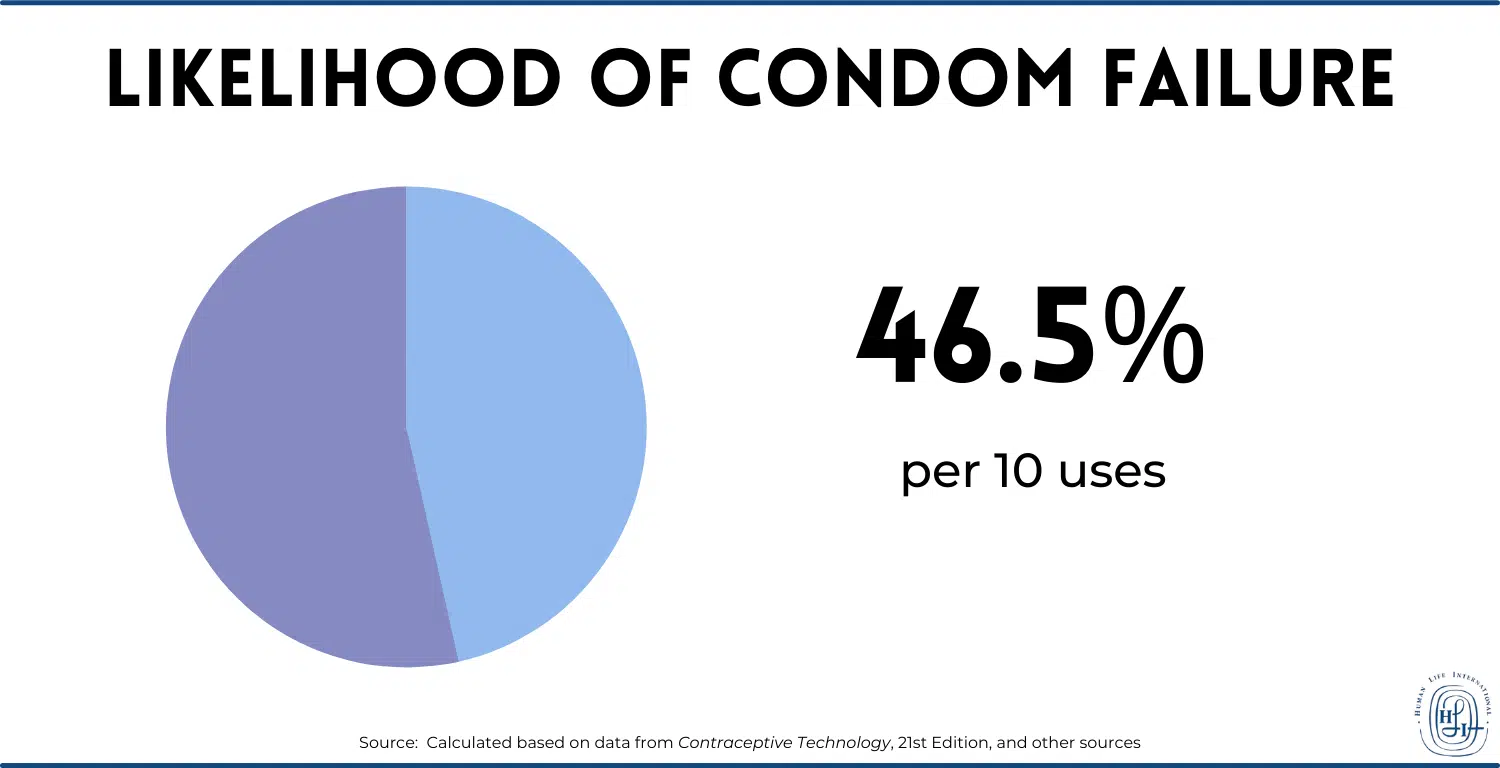
Twenty-three major studies of almost 60,000 condoms used during heterosexual intercourse in five different countries have found that 4% of all the condoms broke and 2.06% of them partially or completely slipped off, for a total “failure” rate of 6.06%. That means that about 1 in 17 uses results in condom “failure.” “Failure” means the possibility of pregnancy (in other words, the marital act may succeed in its natural end despite the interference of the condom). Even the highest-quality condoms used in the most “effective” manner possible by educated, monogamous, adult couples “fail” at a high rate under real-world conditions. This information is available from a Human Life International meta-analysis that draws on information in Contraceptive Technology (21st Edition, 2018) and other studies.2
Correct condom use is uncommon because it is complicated and involves significant attention to detail in moments when one is strongly distracted. A 2012 synthesis of 50 studies on condom use errors identified more than ten potential user errors, in addition to the issues of fit, slippage and breakage that are inherent to the condom itself.3 Several user errors were found to be extremely common, including failure to lubricate the condom (16.0%-25.8% of participants), incorrect withdrawal (43%-57% of condom use events), and incorrect storage (3.3%-19.1% of participants).4
These error rates are recorded from populations in the USA, Canada, and the British Isles, where education about correct condom use is widely accessible.
2. Condoms Do Not “Prevent Pregnancy” over Time
Within a year, 13% of sexually active women whose partners use condoms for contraception become pregnant, according to Contraceptive Technology, 21st Edition, and other top scientific sources. After two years, this means 24% have a pregnancy. After three years, it’s 34%. After four years, it’s 43%. After five years, it’s 50%.5
The bottom line: condoms don’t “prevent pregnancy” in the long run.
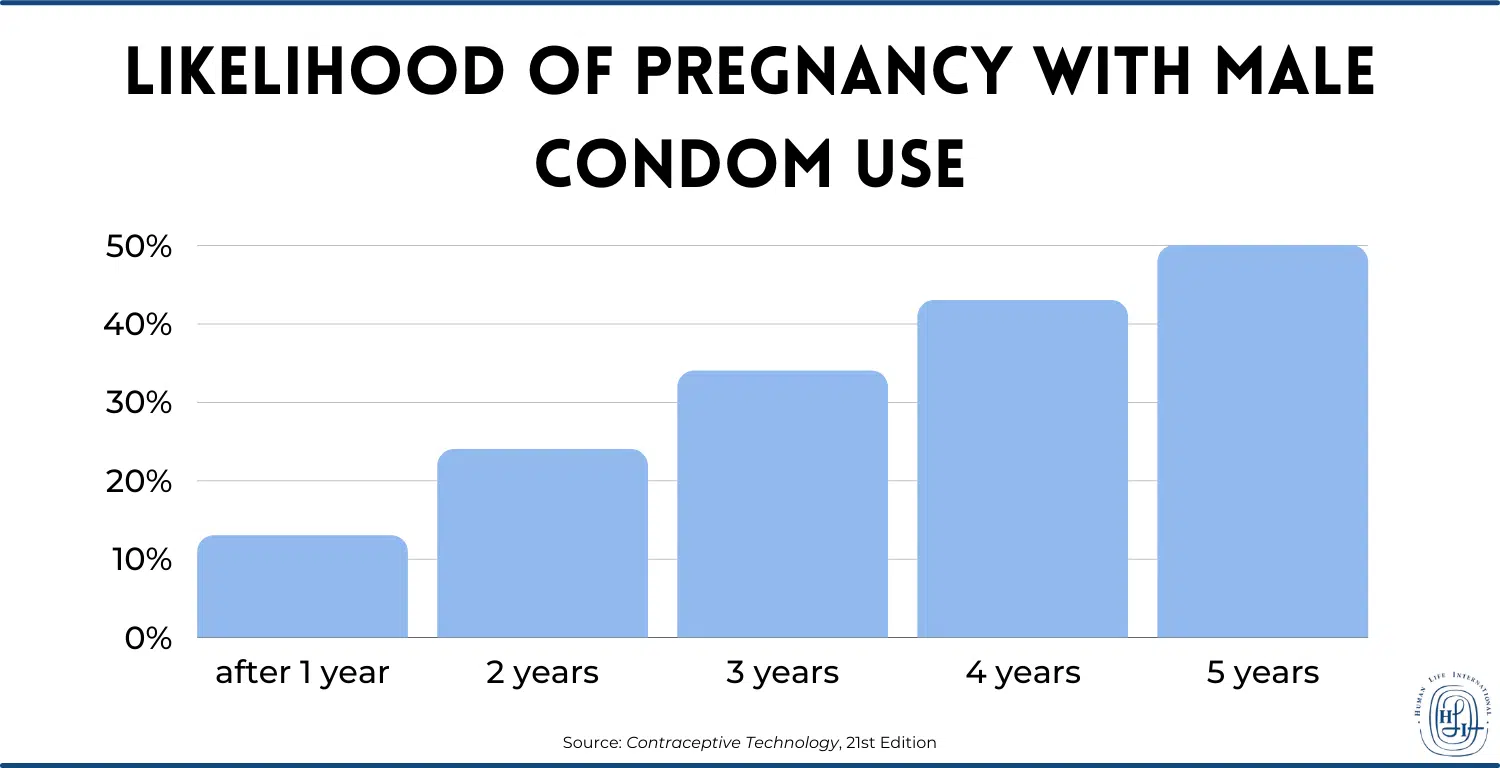
These figures are derived from studies of committed, adult couples using new and properly stored condoms which have not been allowed to degrade. The numbers for youth, for women with multiple partners, and for poor people and those in developing countries using expired or improperly stored condoms are likely worse.
This high “failure” rate means consistent leakage over time, inevitably making many episodes of sexual intercourse with condoms nearly equivalent to sex without condoms.
3. Condom Promoters Use Irrelevant Evidence
The United Nations Population Fund (UNFPA) and other global condom promoters claim that condoms have a 98% “success” rate, instead of the 87% “success rate” documented in real-world studies.
The 98% success rate is based on ideal use every time by well-trained and highly disciplined adults under monitoring by scientists. What is relevant is the “success” rate of condoms by average people, who sometimes fail to put on condoms correctly or replace them immediately if the condom breaks in the heat of the moment, things that happen in the real world over time.

Even studies of trained, committed adult couples using new and properly stored condoms find a real-world “pregnancy prevention success” rate of 87% over a 12-month period (Contraceptive Technology, 21st Edition; same datum as above).6 Unmarried teenagers, often the targets of condom promoters, almost certainly have a far worse record.
4. Ultimately, Condoms Have Failed When Measured by National Statistics
Almost everyone is aware of the massive campaign to promote condom use that has gone on for decades around the world, including the free distribution of condoms by the millions through schools and health clinics in the United States and other Western countries. Obviously, it’s not working.
Teen pregnancy in the United States is still at sky-high levels (there were 171,674 births to mothers aged 15 to 19 in 2019, which of course does not count any pregnancies stopped by abortion or miscarriage, nor births to 10-to-14-year-olds7). There was a decline in teen pregnancies in recent years, probably due to a rise in either chastity or, more likely, other forms of contraception. Additionally, nearly 900,000 abortions are performed each year in the United States as of 2019 (the last year with data reported), a number that is down from previous years but still monumental.8 And given the massive numbers of STIs pervading the United States and the whole world, it’s a safe bet to say condoms haven’t worked for those either.
Conclusion
The main point of this article is that abstinence is important not only from a moral standpoint, but also from a basic scientific and health standpoint. Even disregarding the immorality of condoms for a moment, the fact remains that they can’t even do what they are supposed to do—especially not on the scale of a country’s population. They will not save anyone from the consequences of promiscuous indulgence.

We strongly urge you to look at HLI’s many resources on a wholesome, healthy approach to sexuality, which reserves sex for a fruitful, faithful marriage to one spouse for life.
+ Endnotes
[1] The formula used for this particular calculation was 1 – (1 – 0.0606)n, where n is the number of uses of the condom (so in this case, n=10). The original data is from Robert Hatcher et al., Contraceptive Technology (21st Edition; New York: Ayer Company, 2018), 100.
See also Haishan Fu et al., “Contraceptive Failure Rates: New Estimates From the 1995 Survey of Family Growth,” Perspectives on Sexual and Reproductive Health vol. 31, 2 (March/April 1999): 56–63.
[2] Please contact HLI’s Dr. Brian Clowes, PhD, at bclowes@hli.org to access the meta-analysis raw spreadsheet (F-21-07). It compiles the twenty-three studies’ data.
[3] S. A. Sanders, W. L. Yarber, E. L. Kaufman, et al., “Condom use errors and problems: A global view,” Sexual Health vol. 17, 9(1) (February 2012):81–95.
[4] Ibid.
[5] The “13%” datum is from Hatcher et al., Contraceptive Technology, 100. The formula for calculation of probability is the same as that used already above: 1 – (0.87)n, where n is the number of years (0.87 is the probability of not becoming pregnant in the first year, and so the second year needs a compounded probability, 0.872=0.7569, subtracted from 1; etc.).
[6] Hatcher et al., Contraceptive Technology, 100.
[7] B.E. Hamilton, L. Rossen, L. Lu, and Y. Chong, “U.S. and State Trends on Teen Births, 1990-2019,” National Center for Health Statistics Data Visualization Gallery, 2021.
[8] “Induced Abortion in the United States,” Guttmacher Institute, September 2019.
Related Content
HLI staff writers bring you stories from the mission field and the latest information on life and family issues. All HLI articles are true to Catholic teaching.







I have been using condoms several times a week for nearly 50 years. I have been happily married for 45 years. I have two happy, healthy, wanted, successful, adult children. Their births were carefully, intentionally planned. My wife has a successful career, started after the children were in middle school. One time, a condom broke, and my wife got pregnant- totally unintended. We got an abortion. Though a sad decision, we concluded that another baby at that time would pr0bably have wrecked all of my family’s– including much of our extended family’s lives. This was OUR decision, because we were the only people responsible for it. It affected no one else but ours except for busybody moralists who believe their lives are guided by silly fairy tales. So, condoms worked for us. So there’s much more to condoms than promiscuity. Obviously most pro-lifers are brainwashed or terribly misinformed. I shudder to think of what my family’s lives would be with this unplanned interruption in our lives would have occured. Our belief is that love conquors all, and following dictates of mentally disturbed cultists must be resisted for the truth.
It was a couple of decades ago that an article appeared in the news, stating that barrier contraceptives were responsible, when pregnancy resulted from failure, of an increase in pre-eclampsia about 2.5 times higher than in pregnancies that did not use them. The hypothesis was made that these devices interfere with the development in the woman of the immune response with her male partner that preserves the living fetus. Because the genes from the child are from a male and female, there is disparity between them which could produce proteins that could cause an immune reaction which threatens the health of the mother via pre-eclampsia, which sometimes becomes toxic and deadly. The article made the point that in a normal sexual relationship (monogamous, male/female) the woman’s immune system accommodates to the monogamous husband to protect her from this maladaptive response. We, human beings were made to be exclusively monogamous. The modern sex movement has perverted human nature via birth control of all sorts. Sadly, the greatest victims of this evil movement are those who choose to live according to their human nature, and who often find it impossible to find a chaste spouse.
Thank you for reading and sharing this little-known hypothesis, Gerard.
All forms of birth control are evil and goes against gods will and leads to women becoming irresponsible and promiscuous with multiple sexual partners and it badly hurts not only religious values but also the family unit.
Great points all, Christa. Thank you!
I always knew condoms were unnecessary and even dangerous — this post proves it! I will never allow my children to use them.
This really helped a lot.